BY TYLER DURDEN
Last week, the FDA authorized two much-hyped antiviral treatments for COVID (just in time for Christmas): Merck’s Molnupiravir and Pfizer’s Paxlovid.
Almost immediately after the first data were released, critics were questioning the drugs’ safety profile. But now that the first courses of these “miracle” drugs are finding their way into patients’ bloodstreams, the mainstream media apparently now feels it’s safe to share some of these criticisms with the public.
To wit, NBC News reports that these medications will require “careful monitoring” by prescribing doctors. This could create problems and make doctors more reluctant to prescribe the meds as the omicron-driven winter wave “pummels” America’s supposedly creaking health-care system.
As the omicron surge pummels a pandemic-weary nation, the first antiviral pills for Covid-19 promise desperately needed protection for people at risk of severe disease. However, many people prescribed Pfizer’s or Merck’s new medications will require careful monitoring by doctors and pharmacists, and the antivirals may not be safe for everyone, experts caution.
As a reminder, the FDA only authorized Paxlovid – the Pfizer drug – to treat “mild to moderate” COVID in people as young as 12 who have underlying conditions that raise the risk of hospitalization and death.
Unfortunately, both Pfizer’s and Merck’s drugs come with some serious drawbacks, the biggest being that they can cause life-threatening reactions with widely used medications like statins – taken by people with high blood pressure – blood thinners, and even some antidepressants.
What’s more, the FDA doesn’t recommend Paxlovid for people who have severe liver and kidney disease.
The Merck drug hasn’t even been approved because the experts are worried about potential side effects. Because of this, the FDA has restricted its use to adults, and only in scenarios in which other authorized treatments, including monoclonal antibodies produced by Regeneron and others, are inaccessible or are not “clinically appropriate.”
Here’s a more detailed explanation of how the Pfizer drug works, and why it might be hazardous for some (courtesy of NBC News):
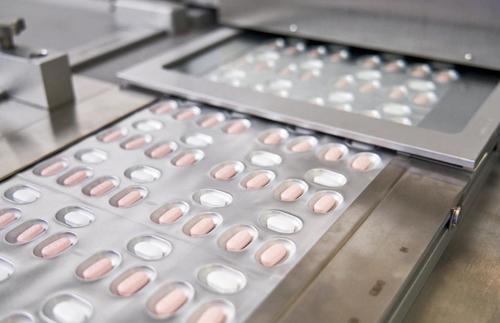
The Paxlovid cocktail consists of two tablets of the antiviral nirmatrelvir and one tablet of ritonavir, a drug that has long been used as what is known as a boosting agent in HIV regimens. Ritonavir suppresses a key liver enzyme called CYP3A, which metabolizes many medications, including nirmatrelvir. In the case of Paxlovid treatment, ritonavir slows the body’s breakdown of the active antiviral and helps it remain at a therapeutic level for longer.
The boosting effect was likely to have been crucial in driving Paxlovid’s high effectiveness in clinical trials.
When Paxlovid is paired with other medications that are also metabolized by the CYP3A enzyme, the chief worry is that the ritonavir component may boost the co-administered drugs to toxic levels.
One expert chimed in to warn that these interactions involving Paxlovid are “not trivial”.
“Some of these potential interactions are not trivial, and some pairings have to be avoided altogether,” said Peter Anderson, a professor of pharmaceutical sciences at the University of Colorado Anschutz Medical Campus. “Some are probably easily managed. But some we’re going to have to be very careful about.”
Supplies of Paxlovid and Molnupiravir are scarce – for now, at least. But the production line is roaring and the two competitors say they hope to produce millions of courses of each medication during the coming year.
We have a question: if a patient dies from an interaction involving a COVID antiviral and their blood pressure medication, would that still be counted as a COVID death?