Education: Pfizer COVID-19 Vaccine Risk Statement (VRS)
This vaccine has not been approved or licensed, and is still under investigation.1DOWNLOAD/PRINT PDF
Pfizer-BioNTech COVID-19 Vaccine:
Short-Term Efficacy & Safety Data










1. WHAT IS THE PFIZER-BIONTECH COVID-19 VACCINE?
The Pfizer-BioNTech COVID-19 vaccine (BNT162b2) is made from synthetic genetic material that is immersed in fatty substances, including cholesterol and polyethylene glycol (PEG). More specifically, modified RNA molecules that encode for a mutated spike (S) protein antigen of the SARS-CoV-2 virus, the virus that can cause COVID-19, are immersed in lipid nanoparticles. The drug is administered in two intramuscular 30 mcg doses, 21 days apart.1
2. HOW WAS THE VACCINE STUDIED PRIOR TO OBTAINING EUA?
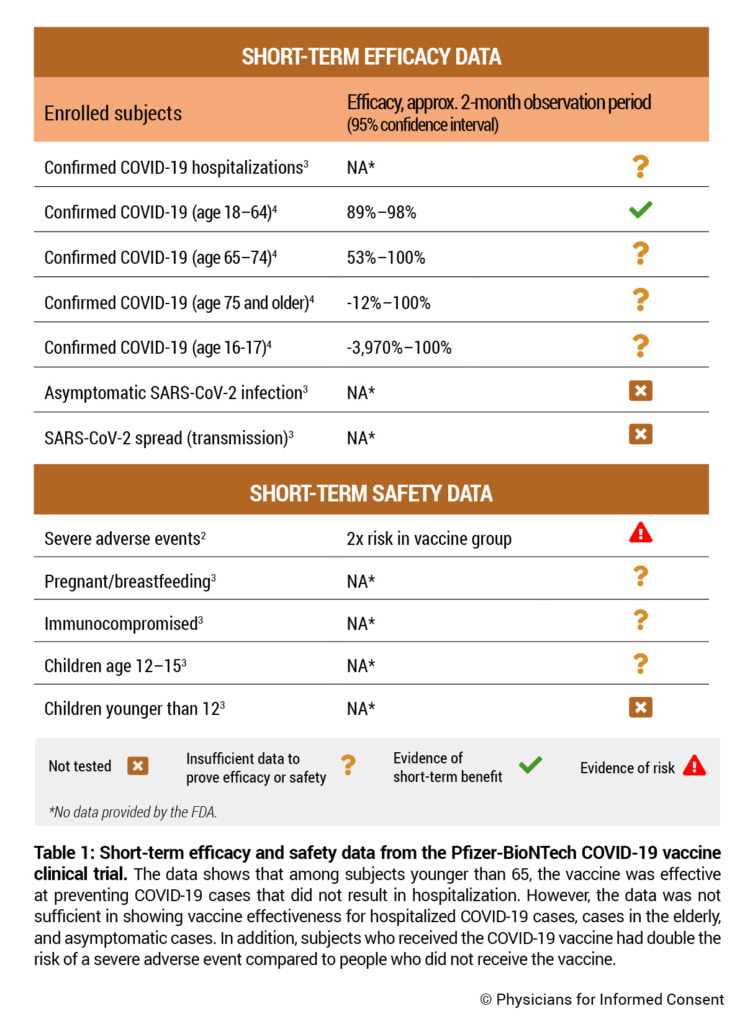
The Pfizer-BioNTech COVID-19 vaccine has obtained emergency use authorization (EUA) from the U.S. Food and Drug Administration (FDA) and is currently investigational.1 The vaccine was studied through nonclinical data from rats and nonhuman primates, and clinical data from humans. The EUA was based on a human clinical trial comparing approximately 22,000 subjects who received the vaccine with 22,000 subjects who did not receive the vaccine (Table 1).2 The trial included a median observation period of two months; 50.6% of subjects were followed up for about two months after the second dose.2 The FDA states that due to the length of the clinical trial’s observation period, “it is not possible to assess sustained efficacy over a period longer than 2 months.”3
3. DOES THE VACCINE PREVENT HOSPITALIZATIONS AND DEATHS?
Since only two hospitalized cases of COVID-19 were observed, the clinical trial did not have enough statistical power to measure the vaccine’s ability to prevent hospitalizations from COVID-19.3 See Table 1. The FDA states, “A larger number of individuals at high risk of COVID-19 and higher attack rates would be needed to confirm efficacy of the vaccine against mortality.”3
4. HOW EFFECTIVE IS THE VACCINE IN ADULTS AND THE ELDERLY?
Vaccine effectiveness was calculated by observing the vaccination status of 178 COVID-19 cases, where a COVID-19 case was defined as the presence of at least one COVID-19 symptom and a positive SARS-CoV-2 test at least seven days after the second dose. In subjects 18 to 64 years old, the vaccine was 89%–98% effective over a two-month observation period.3,4 However, since there were only 15 COVID-19 cases observed in subjects 65 to 74 years old and only five cases in subjects 75 years or older, the clinical trial did not have enough statistical power to accurately measure the vaccine’s effectiveness in those age groups.4 The vaccine may be only 53% effective in subjects 65 to 74 years old and 0% effective in subjects 75 years or older.4 See Table 1. Subjects 65 years or older comprise about 80% of all COVID-19 deaths, and subjects 75 years or older comprise about 60% of all COVID-19 deaths.5
5. IS THE VACCINE EFFECTIVE IN CHILDREN?
Safety and efficacy data was either not tested or insufficient in children younger than 16 years old. In addition, since there was only one case of COVID-19 in subjects 16 to 17 years old, the study did not have enough statistical power to measure effectiveness in that age group.4 See Table 1.
6. IS THE VACCINE EFFECTIVE IN PREVENTING INFECTION WITH SARS-COV-2 OR THE SPREAD OF COVID-19?
The Pfizer clinical trial was not designed to observe asymptomatic infection with SARS-CoV-2 or the effect of the vaccine on the spread (transmission) of COVID-19. Consequently, the FDA states that “it is possible that asymptomatic infections may not be prevented as effectively as symptomatic infections” and “data are limited to assess the effect of the vaccine against transmission of SARS-CoV-2 from individuals who are infected despite vaccination.” Furthermore, “additional evaluations including data from clinical trials and from vaccine use post-authorization will be needed to assess the effect of the vaccine in preventing virus shedding and transmission, in particular in individuals with asymptomatic infection.”3 Approximately 40% of SARS-CoV-2 infections are asymptomatic.6
7. WHAT IS THE RISK OF A SEVERE SIDE EFFECT FROM THE VACCINE?
The Pfizer COVID-19 vaccine clinical trial found the overall incidence of severe adverse events during the two-month observation period to be 1.1%, or 1 in 91, in the vaccinated group and 0.6% in the unvaccinated group, resulting in a vaccine risk of 0.5% or 1 in 200 vaccinated subjects.2 Consequently, subjects who received the vaccine had nearly double the risk of a severe adverse event occurring in the two-month observation period compared to subjects who did not receive the vaccine. See Table 1. A severe adverse event was defined as one that “interferes significantly with participant’s usual function.”7
Of note, approximately 3,400 or 8% of all subjects experienced “suspected COVID-19” because they had symptoms but were not confirmed by testing for SARS-CoV-2; two of these cases required hospitalization, both of which were in the vaccinated group. These cases could represent other influenza-like illness and adverse events; 409 such cases occurred in the vaccinated group within seven days of injection whereas 287 such cases occurred in the unvaccinated group in the same time period. Only the cases that were reported as serious were recorded as adverse events.3 In the clinical trial, only 5% of all illnesses suspected of being COVID-19 were actually found to be COVID-19.
After emergency use authorization for the Pfizer COVID-19 vaccine was obtained and mass vaccination began, the Centers for Disease Control and Prevention (CDC) recorded about 5,000 “health impact events” among 215,000 vaccinated subjects (1 in 43) that, similar to the definition of severe adverse events in the clinical trial, prevented the ability to perform normal daily activities, including work, and required medical attention.8
Additionally, as there were only 11,600 subjects 16 to 55 years of age who received the vaccine,3 and since as of Feb. 2, 2021, about 1 in 31,000 people 15 to 34 years of age contracted a fatal case of COVID-19 in the U.S.,5 the clinical trial does not have sufficient data to determine safety in subjects who are 15 to 34 years of age. Per the FDA, “There are currently insufficient data to make conclusions about the safety of the vaccine in subpopulations such as children less than 16 years of age, pregnant and lactating individuals, and immunocompromised individuals.”3 And, because all subjects were observed for only two months, the long-term safety of the vaccine for any age group is not known.

8. IS THE COVID-19 VACCINE EFFECTIVE AND SAFER THAN COVID-19?
The extent to which the Pfizer-BioNTech COVID-19 vaccine is effective and safer than COVID-19 is not known. The clinical trial indicates that in subjects 65 to 74 years old, the vaccine may be only 53% effective, and in subjects 75 years or older, the age group that comprises about 60% of all COVID-19 deaths, the vaccine may be 0% effective; also, in children age 16 to 17 the vaccine may not be effective. The clinical trial did not have enough statistical power to measure the vaccine’s ability to prevent hospitalizations and deaths, and the trial did not assess if the vaccine prevents asymptomatic infection or spread (transmission) of the virus.
Severe adverse events in the vaccine group occurred in 1 in 91 subjects in the Pfizer clinical trial. The CDC has recorded that 1 in 43 vaccinated subjects was unable to perform normal daily activities and required medical attention. Furthermore, for people 15 to 34 years of age, the clinical trial did not include enough subjects to be able to show that the vaccine is safer than the disease, and because the clinical trial observation period lasted only two months, the incidence of long-term side effects from the vaccine for any age group is not known.DOWNLOAD/PRINT PDF
REFERENCES
- Hinton, Denise M. (U.S . Food and Drug Administration). Letter to: Elisa Harkins (Pfizer Inc.). 2020 Dec 23. https://www.fda.gov/media/144412/download.
- Pfizer. Pfizer-BioNTech COVID-19 vaccine (BNT162, PF-07302048): Vaccines and Related Biological Products Advisory Committee briefing document. Meeting date: 10 December 2020. 2020 Nov 30: 38,46. https://www.fda.gov/media/144246/download.
- U.S. Food and Drug Administration, Vaccines and Related Biological Products Advisory Committee. FDA briefing document: Pfizer-BioNTech COVID-19 vaccine. Vaccines and Related Biological Products Advisory Committee Meeting: December 10, 2020:14,16,17,20,24, 30,31,40,46,48. https://www.fda.gov/media/144245/download.
- U.S. Food and Drug Administration, Vaccines and Related Biological Products Advisory Committee. FDA briefing document: Pfizer-BioNTech COVID-19 vaccine. Vaccines and Related Biological Products Advisory Committee Meeting: December 10, 2020. Table 8: subgroup analyses of second primary endpoint: first COVID-19 occurrence from 7 days after dose 2, by subgroup, participants with and without evidence of infection prior to 7 days after dose 2, evaluable efficacy (7 days) population; 26. https://www.fda.gov/media/144245/download.
- Centers for Disease Control and Prevention. Washington, D.C.: U.S. Department of Health and Human Services. Weekly updates by select demographic and geographic characteristics: provisional death counts for coronavirus disease (COVID-19); [cited 2021 Feb 2]. https://www.cdc.gov/nchs/nvss/vsrr/covid_weekly/index.htm#AgeAndSex.
- Centers for Disease Control and Prevention. Washington, D.C.: U.S. Department of Health and Human Services. COVID-19 pandemic planning scenarios; [updated 2020 Sep 10; cited 2021 Jan 13]. https://www.cdc.gov/coronavirus/2019-ncov/hcp/planning-scenarios.html.
- Pfizer. A phase 1/2/3 study to evaluate the safety, tolerability, immunogenicity, and efficacy of RNA vaccine candidates against COVID-19 in healthy individuals. https://cdn.pfizer.com/pfizercom/2020-11/C4591001_Clinical_Protocol_Nov2020.pdf.
- Clark T. Anaphylaxis following mRNA COVID-19 vaccine receipt. COVID-19 Vaccines Work Group of the Advisory Committee on Immunization Practices (ACIP). Centers for Disease Control and Prevention. 2020 Dec 19; [cited 2021 Mar 16]. https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2020-12/slides-12-19/05-COVID-Clark-508.pdf.
Source… https://physiciansforinformedconsent.org/pfizer-covid-19-vaccine-risk-statement/